|
There are also some approaches that can decrease the amount of "face-down" time. However, there are a number of devices that can make the "face-down" recovery period easier on you. People who are unable to remain in a face-down position for this length of time may not be good candidates for a vitrectomy. If you cannot remain in a face-down position for the required period after surgery, vision recovery may not be successful. What if I cannot remain in a face-down position after the surgery? Changes in air pressure may cause the bubble in the eye to expand, increasing pressure inside the eye. Other less common complications include infection and retinal detachment either during surgery or afterward, both of which can be immediately treated.įor a few months after surgery, patients are not permitted to travel by air. In most patients, a cataract can progress rapidly, and often becomes severe enough to require removal. The most common risk following macular hole surgery is an increase in the rate of cataract development. Because this position can be difficult for many people, it is important to discuss this with your doctor before surgery. Maintaining a face-down position is crucial to the success of the surgery. As the bubble is reabsorbed, the vitreous cavity refills with natural eye fluids. This position allows the bubble to press against the macula and be gradually reabsorbed by the eye, sealing the hole. Surgery is performed under local anesthesia and often on an out-patient basis.įollowing surgery, patients must remain in a face-down position, normally for a day or two but sometimes for as long as two-to-three weeks. The bubble acts as an internal, temporary bandage that holds the edge of the macular hole in place as it heals. In this surgical procedure-called a vitrectomy-the vitreous gel is removed to prevent it from pulling on the retina and replaced with a bubble containing a mixture of air and gas. How is a macular hole treated?Īlthough some macular holes can seal themselves and require no treatment, surgery is necessary in many cases to help improve vision. When a Stage III macular hole develops, most central and detailed vision can be lost. The size of the hole and its location on the retina determine how much it will affect a person's vision. Without treatment, about 70 percent of Stage II macular holes will progress. Without treatment, about half of Stage I macular holes will progress. There are three stages to a macular hole: Are there different types of a macular hole? Reading and performing other routine tasks with the affected eye become difficult. Straight lines or objects can begin to look bent or wavy. In the early stage of a macular hole, people may notice a slight distortion or blurriness in their straight-ahead vision. Macular holes can also occur from eye disorders, such as high myopia (nearsightedness), macular pucker, and retinal detachment eye disease, such diabetic retinopathy and Best's disease and injury to the eye. In either case, the fluid that has replaced the shrunken vitreous can then seep through the hole onto the macula, blurring and distorting central vision. This increases tension on the retina and can lead to a macular hole. Also, once the vitreous has pulled away from the surface of the retina, some of the fibers can remain on the retinal surface and can contract. 
However, if the vitreous is firmly attached to the retina when it pulls away, it can tear the retina and create a macular hole. 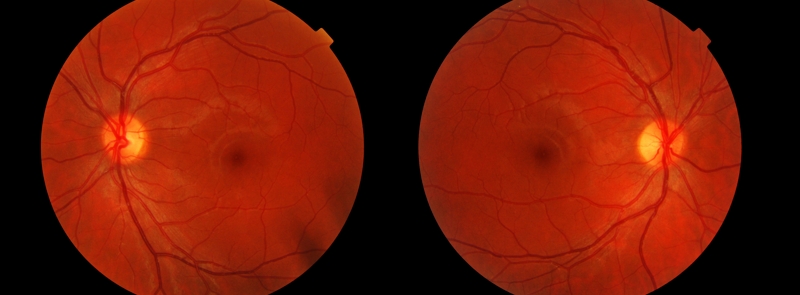
Some patients may experience a small increase in floaters, which are little "cobwebs" or specks that seem to float about in your field of vision. In most cases, there are no adverse effects. Natural fluids fill the area where the vitreous has contracted. 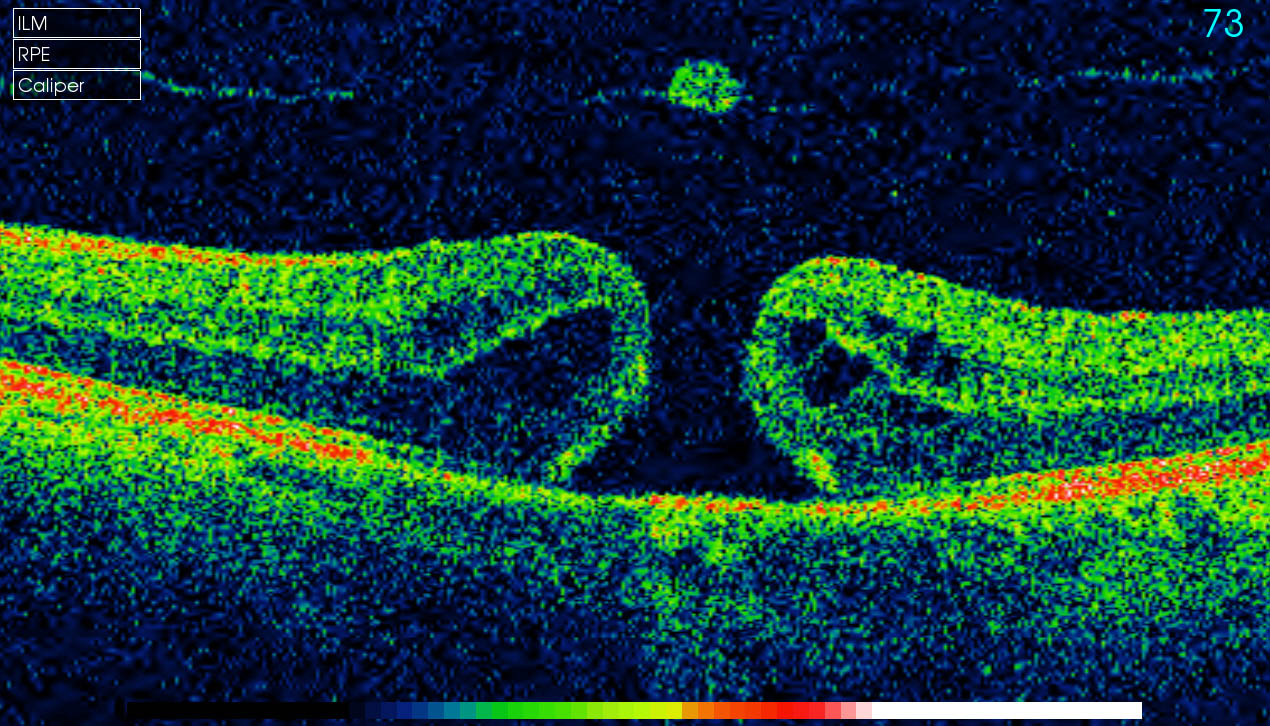
As we age, the vitreous slowly shrinks and pulls away from the retinal surface. The vitreous contains millions of fine fibers that are attached to the surface of the retina. Most of the eye's interior is filled with vitreous, a gel-like substance that fills about 80 percent of the eye and helps it maintain a round shape. Go to the top What causes a macular hole? An eye care professional will know the difference. Both conditions are common in people 60 and over. Macular holes and age-related macular degeneration are two separate and distinct conditions, although the symptoms for each are similar. Is a macular hole the same as age-related macular degeneration? Macular holes are related to aging and usually occur in people over age 60. The macula provides the sharp, central vision we need for reading, driving, and seeing fine detail.Ī macular hole can cause blurred and distorted central vision. A macular hole is a small break in the macula, located in the center of the eye's light-sensitive tissue called the retina.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
